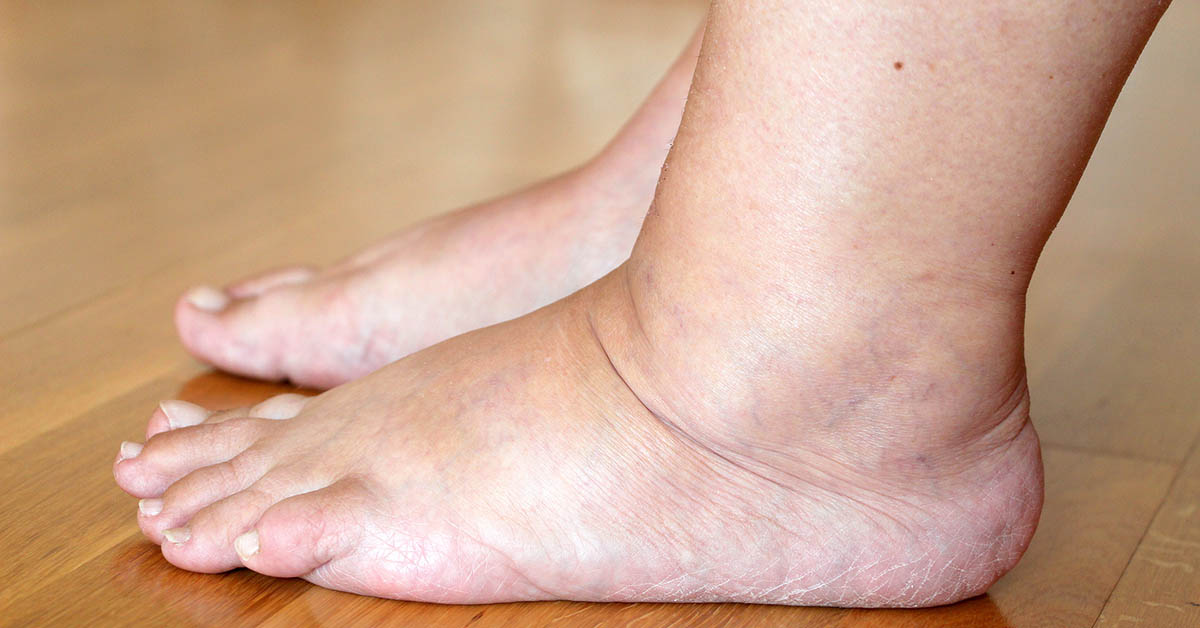
Most of us have experienced swelling, often because of a twisted ankle or some other type of injury.
Typically, swelling is temporary and fades through the healing process, but for people with a condition known as lymphedema, swelling can be a chronic, life-altering challenge.
Unlike swelling associated with an injury, which is known as edema, lymphedema is caused by a disruption in the body’s lymphatic system that results in a buildup of protein-rich lymph fluid.
Lymphedema is commonly associated with cancer treatments that damage lymph nodes or require lymph node removal. But it can also be hereditary or result from vein and circulatory conditions, obesity and infections.
“Think of it like a swimming pool,” says Amy Parker, a clinical specialist and physical therapist at Tidelands Health Rehabilitation Services at Murrells Inlet who specializes in treating the condition. “In the case of cancer treatments, you may be removing some of the filters in the pool, which can cause things to back up.”
In other cases, imagine the pool overfilling due to a storm or hurricane, she adds.
A lifelong challenge
Lymphatic swelling is sometimes mistaken for edema, which can delay treatment. Diuretic medications can make lymphedema worse by removing water and causing lymph fluid to concentrate more.
Untreated, lymphedema-related swelling can restrict movement, increase the risk of infection from wounds and lead to a thickening of the skin known as fibrosis. In extreme cases, the fluids that build up can leak from your skin.
“It can really disrupt quality of life,” Parker says. “Often, patients are embarrassed. I have patients that can barely wear shoes.”
Featured Article
‘I couldn’t wear jeans’ | Pawleys Island woman finds relief from painful swelling
Read ArticleAlthough there’s no cure for lymphedema, the condition can be managed to help limit symptoms and reduce the risk of complications. If you’re struggling with the condition, speak to your physician or other qualified care provider, who can refer you to a physical therapist like Parker.
Physical therapy for lymphedema includes lymphatic massage, which gently helps move the pooling fluid from swollen areas back into the torso where most of the lymphatic system resides.
Treatment may also include the use of compression garments, such as stockings and sleeves, or a compression pump, which applies constant pressure to keep lymphatic fluid from pooling in affected areas. Compression garments need to be worn during the day and can be removed at bedtime. Parker recommends buying medical-grade garments that are tailored to fit your body’s measurements.
Activity is vital
Because the lymphatic system depends on your muscles for pumping, moving your body provides a crucial component of treatment, Parker says. Going for a walk, which may be difficult with a swollen leg or ankle, can be enough to get the system moving the way it should.
Enjoying this story? It’s free to republish. Learn more.
“You get more bang for your buck when you take a walk with compression socks on,” Parker says.
Along with those treatments, Parker recommends her patients take special care of their skin and fingernails using a low-pH lotion to help limit the risk of infection.
Ultimately, the goal of physical therapy is to help patients with lymphedema manage the condition independently and regain quality of life, Parker says.
“Every patient leaves with the pieces of that puzzle to help manage themselves,” she says.