Sept. 8, 2020 is not a day Heather Gainey will soon forget. That Tuesday, she got some much-welcomed news: She was cancer-free.
Gainey, 42, was diagnosed with a particularly aggressive form of breast cancer six months earlier on March 2. She underwent 14 rounds of chemotherapy prior to a lumpectomy on Aug. 31. The tissue and lymph nodes that were removed during the surgery showed no signs of cancer, meaning the chemotherapy had achieved its intended purpose.
“It sounds crazy, but I like to say I’m the luckiest girl ever to have cancer,” says Gainey, who lives in Myrtle Beach. “I quickly had an army of friends and great family for support. And my doctors were so wise and treated me like their family. They developed a plan for me and just knocked it out of the park.”
Innovative treatment approach
Gainey says her cancer treatment was done “backwards” since she had chemotherapy prior to her lumpectomy to remove the cancerous tissue. Called neoadjuvant treatment, Gainey received several chemotherapy medications intended to weaken or kill cancer cells before her lumpectomy.
Dr. Craig Brackett, medical director of the Tidelands Health breast health program and Gainey’s surgeon, says patients who come to Tidelands Health for cancer treatment benefit from an individualized approach to care based upon each patient’s unique circumstances.
The Tidelands Health Cancer Care Network, a collaboration with MUSC Health, is our region’s most comprehensive provider of cancer care.
“When you receive a cancer diagnosis, you need the best team, technology and treatments to fight the disease,” says Dr. Brackett. “At Tidelands Health, we bring together a multidisciplinary care team to offer each patient an integrated, personalized approach to treatment.”

Gainey was an ideal candidate for neoadjuvant treatment, which is when chemotherapy takes place before cancerous tissue is surgically removed.
As a node-positive patient, Dr. Brackett says Gainey was the “perfect candidate” for having neoadjuvant treatment. That’s because patients with advanced or aggressive breast cancer that has spread to the lymph nodes often have better outcomes when chemotherapy is conducted prior to the surgical removal of the cancerous tissue.
“There are multiple advantages to giving chemo before surgery,” says Dr. Brackett, who practices at Tidelands Health Breast Center, our region’s only surgical practice dedicated solely to breast health. “The data shows you’ll be able to tell if the chemo is working before you do surgery, and you’ll be able to kill circulating tumor cells.”
Sign up today for ‘In The Pink’ Breast Cancer Awareness Walk
Show your support for breast cancer survivors by signing up today for the 15th annual “In The Pink” Breast Cancer Awareness Walk, which is continuing throughout the month of October, by clicking here.
Additionally, patients who might have otherwise had a mastectomy can often opt for breast conservation therapy, he says.
That’s exactly what happened in Gainey’s case. She was able to forego a mastectomy, instead receiving a combination of medications meant to kill the cancer in her breasts and lymph nodes.
“I have no doubt it was the right plan. I never felt the need for a second opinion, and it was clearly the right approach,” she says.
Close to home
Gainey says she’s lucky she was able to stay close to home for her cancer treatment. Her care team was led by Dr. Brackett and Dr. Sara Adams, an experienced oncologist who provides care at the Murrells Inlet and Georgetown locations of Tidelands Health Oncology.
“My husband and I didn’t have to pack up our family and leave to go find such amazing doctors,” says Gainey, who owns a nail salon and has five children, including a 2-year-old. “Our community is so blessed to have these resources right here.”
As is often the case during cancer treatments, Gainey had to overcome challenges during the treatment process. For example, her body didn’t respond well to some chemotherapy medications, so adjustments had to be made along the way.
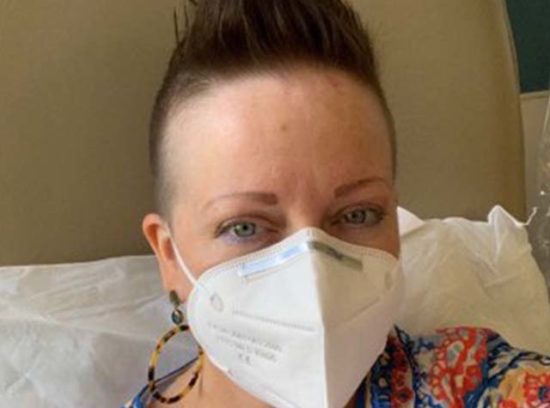
Gainey didn't get too concerned about losing her hair as a result of cancer treatment. When it started thinning, she styled it into an upswept coiffure then, when it was time, she shaved it all off.
Even so, Gainey’s weight remained stable, her immune system strong and her appetite good.
She really wasn’t all that concerned about losing her hair, either. “For me, I had a lot of fun with my hair,” she says.
When it started thinning, Gainey styled it into an upswept coiffure, somewhat reminiscent of a mohawk. When it was time, she shaved it all off.
“Fortunately, my head was pretty decent looking,” she says with a laugh. “It was actually very freeing not to have hair.”
Even though Gainey’s cancer is gone, she will receive infusions of the medication Herceptin three times a week until May. She’ll also have radiation daily for several weeks.
“The Herceptin and radiation are used as precautions,” she says. “Those will be the two things that I do next, and hopefully that’s it.”
Sharing her journey
Gainey says she believes it’s important to share her story, especially with people who are newly diagnosed. She frequently writes about her experiences on social media, and when she returns to the infusion floor, she welcomes the chance to offer advice and prayers for patients just setting out on their cancer treatment journeys.
“Being positive and having a 2-year-old through all this is definitely a battle. I try to encourage people that I talk to now and tell them they’re going to have highs and lows. You have to go through all of them, but you can’t get stuck there,” she says.

Gainey says a positive attitude is key in the battle against cancer.
Dr. Brackett says a positive outlook is required both on the part of the patient and the physician.
“It helps to be positive, and it helps to have physicians present information in a way that gives patients hope. Patients need to see they are supported so they can maintain good mental health and a positive attitude,” he says.
For Gainey, a strong support system and feeling confident in her treatment plan helped her maintain an optimistic view.
“I’ve been lucky, I really have. I’ve learned you have to take one day at a time and count your blessings. That’s how you beat this,” Gainey says.






