For years, finger sticks were the primary method for people with diabetes to check their blood glucose levels.
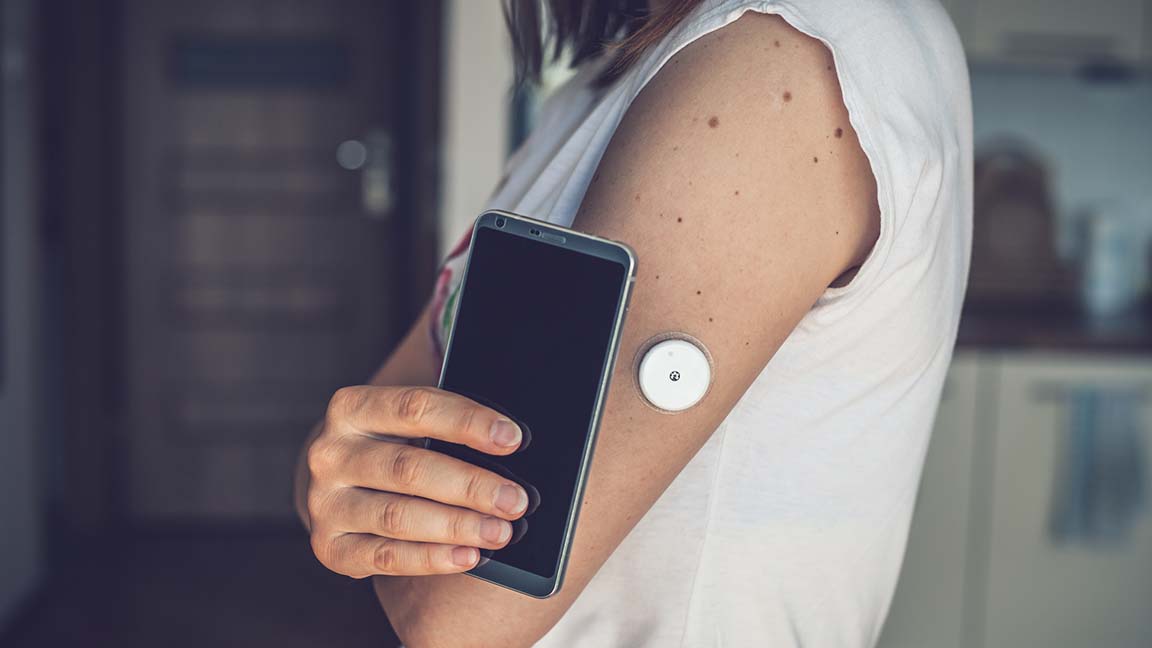
The advent of new technology known as continuous glucose monitoring (CGM) is fundamentally changing the process for many people. CGM devices use implantable or wearable patch sensors that read blood sugar values and can alert patients of high or low blood sugar.
“They can be used to make therapeutic decisions and guide management of the disease,” says Tidelands Health endocrinologist Dr. Gauri Dhir, a board-certified, fellowship-trained physician who offers care at Tidelands Health Endocrinology in Myrtle Beach. “Sensors have changed the way diabetes is being managed.”
Fewer fingerstick tests
Before CGM became available, patients had to rely on an A1C test, which provides a picture of someone’s average of blood sugar levels over the previous two to three months, and frequent fingerstick tests.
Although people with diabetes still need to undergo A1C testing, CGM devices improve management of the disease by providing glucose readings in real time and recording data that shows trends and patterns. The devices can also reduce or even eliminate the need for a patient to prick a finger to measure blood sugar levels.
Featured Article
Too little sleep among children linked to higher risk of Type 2 diabetes
Read Article“Because CGM provides real-time information about blood glucose levels, the technology has given patients more accountability and enables them to more actively engage in their diabetes management and care,” Dr. Dhir says. “It has a true positive impact on behavioral modification and patient engagement.”
In addition to alerting an individual about the need to eat or administer insulin to maintain proper blood sugar levels, some CGM devices are worn in combination with a pump that delivers insulin, if needed, based on data from the device.
Insulin is a peptide hormone that helps the body regular blood sugar levels. Patients with Type 1 diabetes have trouble producing enough insulin. People with Type 2 diabetes can produce insulin but are unable to use it effectively.
It’s critically important to properly manage blood sugar levels because low (hypoglycemia) or high blood sugar (hyperglycemia) levels can cause damage to the body’s organs or be life threatening.
“This technology has lessened the burden overall in managing a patient’s diabetes for those who are comfortable and ready to use it,” Dr. Dhir says.
How CGM works
There are several CGM devices on the market. Some require the user to wear a sensor patch held in place on the skin with adhesive, while others use an implantable sensor under the skin. Most devices take readings every five minutes and require replacement of the sensors every 10 to 14 days, depending on the device. Implantable devices are changed every six months in a care provider’s office.
Enjoying this story? It’s free to republish. Learn more.
Readings are captured by the sensor and sent wirelessly via transmitter wirelessly to a receiver similar to a cell phone, to an app on a smartphone or to an insulin pump.
Some patients are uncomfortable using the devices, often because of the need to learn and manage the technology, Dr. Dhir says. Although individuals are taught how to use the equipment before beginning to use it, the challenge of working with the technology can be understandably be overwhelming for some users, she says.
Others report being self-conscious because the device may be visible to others or because the devices are not convenient to wear when playing contact sports or engaging in water exercise.
Valuable tools
Although CGM devices aren’t a cure for diabetes, they have become a valuable tool for managing the disease and helping patients take a more active part in their own care, Dr. Dhir says. And for the physicians caring for people with diabetes, the devices provide a bigger picture of how the disease is affecting their patients so they can customize care as needed.
“Real-time glucose monitoring gives us glucose trends, which helps us identify patterns to prevent complications,” Dr. Dhir says. “It also allows for remote monitoring and management, saving a lot of time during clinic visits.”
Once a patient becomes comfortable using the machine, it can add to their quality of life.
“Patients aren’t burdened by always thinking about their blood sugar if the CGM device is continuously monitoring and recording data for them,” Dr. Dhir adds. “This can give a patient peace of mind as they go about their daily lives.”

Dr. Gauri Dhir
Endocrinologist, Tidelands Health Endocrinology
Call to Schedule
Bio
Dr. Gauri Dhir is a board-certified physician who provides a range of care to treat diabetes, obesity, thyroid disorders, osteoporosis and adrenal and pituitary disorders.
Learn MoreMedical Education
Education
Punjabi Government College
Residency
Thomas Jefferson University Hospital, Internal Medicine
Internship
Yale – Griffin Hospital, Internal Medicine
Fellowship
Temple University, Endocrinology
Awards
- Board Certified – ABIM- Internal Medicine 2007
- Board Certified -ABIM- Endocrinology Diabetes and Metabolism 2012
- Endocrine Certification in Neck Ultrasounds (ECNU) 2014
- Certified Clinical Densitometry CCD -2017
- Certified Eversense Specialist – Implantable Sensors 2019
Meet the Expert
Dr. Gauri Dhir
Call to Schedule
Dr. Gauri Dhir is a board-certified physician who provides a range of care to treat diabetes, obesity, thyroid disorders, osteoporosis and adrenal and pituitary disorders.